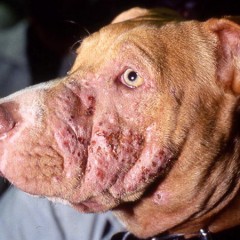
 Staphylococcal Pyoderma Bacteria of the genus Staphylococcus are gram-positive cocci that exist as part of the normal cutaneous flora of mammals. However, due to a disruption in the skin’s natural defense mechanisms, these bacteria can proliferate and cause infection. Dogs harbor coagulase-positive staphylococcus on non-lesional skin and mucosal surfaces (carriage sites). Studies have shown that such carriage sites may be the source of pathogenic staphylococcus in dogs, resulting in the lesions of bacterial folliculitis. Pyodermas are extremely common in veterinary medicine. Staphylococcus intermedius is the most common bacterial skin pathogen in dogs and cats. Most cases are secondary to hypersensitivities (atopy, food allergy, flea allergy dermatitis), endocrinopathies (hypothyroidism, hyperadrenocorticism), or ectoparasitic infestation (demodicosis, sarcoptic mange). The depth of involvement of pyoderma is classified as surface, superficial, or deep. Surface pyodermas consist of superficial dermal erosion, the most common of which include skin fold pyoderma and pyotraumatic dermatitis (hot spots). Superficial pyodermas involve bacterial invasion into the hair follicle (folliculitis) and microabscessation of the epidermis. The unifying lesion of superficial bacterial pyoderma/folliculitis is the folliculocentric pustule. However, pustules are transient and rupture easily, resulting in the formation of crusted papules and/or epidermal collarettes. In the condition known as superficial spreading pyoderma (SSP), pustules evolve into coalescing and expanding erythematous macules. As these macules expand, superficial keratin layers lift and peel peripherally, resulting in expansive epidermal collarettes. The collarettes in SSP are more prominent than in folliculitis, and pustulation is less evident. Bacterial folliculitis and SSP may coexist, though one form usually predominates. The most common presentation of feline bacterial folliculitis is miliary dermatitis. If the bacterial infection extends beneath the hair follicle, the disease is termed deep pyoderma. Lesions of deep pyoderma include furunculosis (ruptured hair follicles), nodules, and/or draining tracts.
Surface
Deep
Superficial Bacterial Folliculitis:
Methicillin-resistant Staphylococci Methicillin-resistant staphylococci are identified on laboratory reports as having an MIC for oxacillin = 2 µg/mL. Oxacillin is used in susceptibility tests as it provides more accurate results. However, the resistant organisms are termed “methicillin-resistant”, resulting in confusing terminology. In veterinary medicine, methicillin resistance amongst staphylococci isolated from domestic animals has been documented since the 1970s. The first isolates of methicillin-resistant Staphylococcus aureus (MRSA) were reported from mastitic cows. Since then MRSA has been identified in dogs, cats, horses, sheep, pigs, and chickens. The prevalence of MRSA infections in domestic animals is difficult to estimate. A recent survey found that MRSA infections were most prevalent among canine and equine patients (Middleton et al 2005). In a study conducted at the University of Pennsylvania Veterinary Teaching Hospital, the frequency of methicillin-resistant infection by S. aureus, S. intermedius, and S. schleiferi was determined (Morris et al 2006). Rates of methicillin resistance were: S. aureus 35%, S. intermedius 17%, and S. schleiferi 40%. Frequency of MRSA isolation from dogs and cats was similar, though methicillin-resistant S. intermedius (MRSI) and methicillin-resistant S. schleiferi (MRSS) were more common in dogs. MRSS was usually associated with superficial skin and ear infections and MRSA was more commonly associated with deep infections. Recently, a study was conducted among attendees at an international veterinary conference. MRSA was isolated from the nares of 6.5% attendees, with colonization more common for large-animal than small-animal personnel (Hanselman et al 2006). Staphylococcus aureus MRSA has been increasingly recognized as a problem in both human and veterinary medicine. Methicillin was first introduced in human medicine in the late 1950s and was used to treat penicillin-resistant staphylococcal infections. Methicillin-resistance was reported by 1961. Today, more than 90% of human isolates produce penicillinase. Although this low-level resistance can be overcome by administration of a “protector” (i.e. clavulanic acid), high-level resistance involves production of a penicillin binding protein that cannot be overcome by a protector molecule. MRSA strains are resistant to ß-lactams, with resistance mediated by the mecA gene. The mecA gene encodes for a penicillin-binding protein (PBP2a) expressed in the bacterial cell wall. This gene confers intrinsic resistance to all ß-lactam antibiotics. As such, these antibiotics are ineffective and should be avoided. Also, most MRSA isolates are resistant to other classes of antibiotics, thus displaying multi-drug resistance. Indeed, antibiotic use in patients with a methicillin-resistant strain may be a risk factor for development of resistance to other categories of antimicrobials. Some evidence exists that MRSA became methicillin resistant from coagulase-negative staphylococcal strains (Robinson and Enright 2004). Risk factors in humans include prolonged antimicrobial therapy, surgery, prolonged hospitalization, and contact with other infected patients or carriers. In animals, MRSA infections are associated with post-operative infections, open wounds, the presence of implants (suture, orthopedic implants), contamination of the hospital environment, and contact with infected or carrier humans. In humans, carriage sites of S. aureus include the anterior nares, throat, axilla, perineum, and groin. The skin is often colonized by S. aureus in nasal carriers and transmission is considered to occur by hand contact. As such, elimination of nasal carriage-by use of topical mupirocin-will also eliminate hand carriage. For many years, MRSA has been considered a healthcare-associated pathogen (hospital-acquired MRSA; HA-MRSA). However, infections are now appearing in healthy individuals in the community without healthcare-associated risk factors (community-acquired MRSA; CA-MRSA). Recent evidence strongly suggests that animals become colonized with MRSA through contact with either colonized or infected humans-a “reverse” zoonotic phenomenon. These animals can thus serve as a reservoir for human re-infection or re-colonization. Measures to prevent and control MRSA in humans have been widely published. Such information can be obtained by the Centers for Disease Control (www.cdc.gov). No evidence- based research has been conducted on control measures in animals, although specific institution-based guidelines have been established (Nutall 2006, Weese 2006). General guidelines include hand hygiene, barrier protection (gloves, gowns, disposable masks) when dealing with wounds, aseptic technique during surgery, and disinfection of surfaces/equipment between patients. Although identification of colonized or infected animals and veterinary staff would be ideal, such routine screening is not practical. However, identification of MRSA infection in suspect cases is important. Samples for bacterial culture should be collected from animals with non-healing wounds, non-antibiotic responsive infections, and animals from known MRSA-positive households. This may be expanded to animals belonging to healthcare workers or other at-risk occupations. Staphylococcus intermedius Staphylococcus intermedius can be associated with dog bite infections in humans, and there has been a single case in a human patient with otitis externa (Tanner 2000). However, the overall risk of S. intermedius causing disease in humans is rare. A potential risk does exist if there is a transfer of resistant genes from antimicrobial-resistant S. intermedius to human pathogenic staphylococci (i.e. S. aureus). The occurrence of antimicrobial-resistant S. intermedius strains was investigated in 13 dogs affected by deep pyoderma and their owners (Guardabassi et al 2004). Isolates of the dog-owner pairs were typed and results showed that 46% of owners carried strains genetically identical to those isolated from their dogs. Strains were resistant up to five different antimicrobial classes. Although the direction of transmission was not investigated in this study, the fact remains that S. intermedius is a normal inhabitant of dog skin and rare in humans. Thus, it is possible that transmission occurred from dogs to humans. Staphylococcus schleiferi and Coagulase-negative Staphylococcus Recent studies have revealed that coagulase-negative staphylococci are implicated in a number of significant infections in humans and companion animals. Coagulase-negative staphylococci have historically not been considered to be pathogenic in companion animals. Coagulase-negative trains are a major component of normal cutaneous flora. However, if the skin has been damaged by trauma, mechanical disruption (needles, catheters), or direct implantation (prosthetic implants), these organisms can cause opportunistic infection (Kloos and Bannerman 1994). Many of these pathogens have shifted toward the more antibiotic-resistant strains. Current antibiotic practices, including pre-operative antibiotic prophylaxis and therapeutic use of cephalosporins have led to the selection of these antibiotic resistant strains (Dancer 2001). Staphylococcus schleiferi was first identified in the external auditory meatus of dogs with external otitis in 1990. S. schleiferi can be either coagulase positive (subsp coagulans) or coagulase negative (subsp schleiferi). In dogs, infection with S. schleiferi may be associated with prior antibiotic use (Frank et al 2003). Methicillin-resistance has recently been described in S. schleiferi subsp. coagulans and has been shown to be due to the presence of a mecA gene. Treatment Treatment of superficial bacterial folliculitis is commonly based on empiric selection of antibiotics. Cephalosporins, such as cephalexin and cefpodoxime, remain the mainstay of empiric treatment among veterinary dermatologists. Clindamycin also has excellent efficacy against staphylococcus and is often used for initial treatment. However, clindamycin’s use in recurrent pyoderma can be limited by development of resistance. When empiric treatment is not successful, bacterial culture and susceptibility testing may be indicated. The following general treatment guidelines should also be considered:
When dealing with methicillin-resistant strains, avoid the use of all beta-lactam drugs! This includes pencillins, cephalosporins (all generations), cephamycins, carbapenems, and amoxicillin-clavulanic acid. Erythromycin and clindamycin should only be used if both drugs are susceptible. Also, many MRSA strains isolated are also resistant to fluoroquinolones. Fluoroquinolones and Fluoroquinolone- Resistance Fluoroquinolones (FQ) are NOT broad-spectrum antibiotics and should not be considered as such. They are not effective against anaerobes, have variable efficacy against streptococcus, and only “good” efficacy against staphylococcus. FQ resistance in S. aureus results from genetic mutation. Previous FQ use is one of the most important risk factors for FQ resistance and evidence exists that use of fluoroquinolones may result in methicillin resistance. Even a single dose of a FQ has been associated with changes in the resistance pattern of commensal coliforms in human patients. Over the past several years, there has both been an increased use of FQs and an increased incidence of methicillin resistance. Some S. aureus strains are capable of expressing resistance to both methicillin and FQ. This would be especially advantageous in an environment of abundant FQ use. The use of FQ with low potency for S. aureus may lead to a higher colonization in individuals with methicillin resistant strains (Venezia et al 2001). This is supported by the fact that countries that rarely utilize FQ also have a very low incidence of MRSA (Shopsin et al 2000). Fluoroquinolones influence methicillin resistance by selective inhibition of more susceptible subpopulations in heteroresistant S. aureus (Venezia et al 2001). Thus, surviving populations are more resistant to both methicillin and FQ. Ciprofloxacin is now generic and this is reflected in decreased cost. However, it is extremely important to remember that enrofloxacin is converted to ciprofloxacin after oral dosing. Also, the bioavailability of enrofloxacin is nearly twice that of ciprofloxacin. Thus, if ciprofloxacin is used, the dose must be double the enrofloxacin dose to achieve therapeutic efficacy. So, based on concerns of antibiotic resistance patterns and judicious antibiotic use, I only use FQ on two occasions: 1) deep pyoderma (i.e. German shepherd dog pyoderma, furunculosis) and 2) necessity based on culture and susceptibility results. The minimum dose I start with is 10 mg/kg of enrofloxacin (see discussion of concentration dependent drugs later). This would translate to 20 mg/kg of ciprofloxacin to account for the decreased bioavailability. When to culture Culture and susceptibility testing is one of most important guides in antimicrobial selection. Cultures should always be obtained for life-threatening infections. In general, I elect to culture under the following guidelines: 1) non-antibiotic responsive pyoderma, 2) history of multiple antibiotics used in the past, 3) recurrent pyoderma, 4) suspicion of underlying systemic or endocrine disease, 5) known at-risk environment. Remember, performing a culture is never a BAD idea. What to culture Intact pustules are the lesion of choice to culture in superficial pyoderma. However, due to their fragile nature, pustules are often not present. In these cases, epidermal collarettes may be sampled by lifting up the edge of the collarette and using a sterile culturette to swab underneath, or by rolling a culturette across the collarette (White 2005). A skin biopsy using a standard biopsy punch may also be submitted for aerobic culture. If a skin biopsy is chosen, it is necessary for the animal to be lightly sedated, as lidocaine can inhibit bacterial growth. In cases of superficial pyoderma, lesions do not need to be scrubbed prior to sampling or biopsy. A biopsy and pre-biopsy scrub should always be performed in the case of deep pyoderma or draining tracts. Preventing resistance Previous antimicrobial therapy is one of the most important factors associated with resistance. As previously stated, the principal risk factor for FQ resistance is previous FQ use. Also, the wide use of cephalosporins may also be a strong contributing factor for the development of MRSA (Dancer 2001). Thus, preventing resistance is a responsibility veterinarians must take seriously. The development of infection despite recent or current antibiotic therapy indicates that the organism is resistant to the antibiotic chosen, or is perhaps due to an inappropriate dosing regimen. Preventing resistance must be a concerted effort of judicious antimicrobial use coupled with proper administration tactics. The first step in judicious antimicrobial use is confirming the need. Although it is common-place to think of antibiotic administration as a “do not harm” scenario, antimicrobial administration in the absence of infection can lead to serious long-term ramifications. One of the best diagnostic tools we have in “confirming need” is to conduct surface cytology and look for the presence of bacteria. The second step is identifying the target site of action (in this case, skin) and knowing the pharmacodynamics and pharmacokinetics of the drug (or, can it get to the target site). Quite possibly, the single most important action that can be taken to minimize resistance is to ensure that adequate drug concentrations are reached at the site of infection. Organisms must be exposed to maximum drug concentrations for a sufficient time period. Doses should be maximized in order to ensure that a Cmax: MIC of 10 or more is achieved for concentration-dependent drugs (i.e. fluoroquinolones) and the proper dosing interval should be used for time-dependent antibiotics (plasma drug concentrations should be above the MIC for the majority of time). TAKE-HOME POINTS:
Click here to download a copy of this information in Adobe PDF format Comments are closed.
|
AuthorDr. Joseph A. Bernstein, DVM, DACVD
In addition to small animal and equine cases, Dr. Bernstein continues to publish research and acts as a consultant for zoos and research centers for the benefit of exotic animals and nonhuman primates. |

 RSS Feed
RSS Feed